Diarrhoea
Most HIV drugs list diarrhoea as a possible side effect.
In practice, this is now less common. If it does occur it is generally mild and short term.
Don’t be worried about talking to your doctor. Otherwise it will not be treated properly. It can be a symptom of other health problems not related to HIV.
Diarrhoea can be related to something you have eaten, other infections and travel to other countries.
Diarrhoea includes both:
- Looser and more watery stool.
- Needing to go to the toilet more often.
Moderate or severe diarrhoea can lead to dehydration, poor absorption of nutrients and drugs, weight loss and fatigue.
Long-term diarrhoea and heavy alcohol use can damage the pancreas. This can upset the production of enzymes from the pancreas that help you digest food, and cause diarrhoea.
Most of us get diarrhoea at some point and having a lower CD4 count increases this risk. So HIV can cause diarrhoea with a low CD4 count. Most diarrhoea is self-limiting lasting just for a few days. However, sometimes it can last for a few days, weeks, months or, in some cases, years.
Anything lasting more than a few days is serious enough to talk to your doctor about.
If HIV meds continue to cause this side effect, it is probably better to try another HIV drug.
How to describe diarrhoea to your doctor
- How often each day do you need to use the toilet?
- How loose is your stool? Is just less firm or is it completely watery?
- Is this linked to certain times of the day or after eating certain foods?
- How urgently do you need to use the toilet?
- Has this affected your social life in terms of going out?
- Do you feel more tired or weak as a result?
Finding the cause
Often diarrhoea is temporary and may be due to starting or changing treatment. Symptoms often reduce within a few days or weeks as you get used to the HIV drugs.
In this case, short courses of anti-diarrhoea medications such as loperamide (Imodium) or diphenoxylate and atropine (Lomotil) can work.
If diarrhoea persists for more than a few days, and is not directly linked to starting a new combination, it is important to run tests to check that it is not being caused by bacterial or parasite infections.
A short course of antibiotics will usually clear any infection, and can be prescribed where an infection is suspected but cannot be isolated.
Heavy alcohol use, or the class of HIV drugs called nukes (NRTIs) can also change the way your body responds to diarrhoea. This can be checked by testing a stool sample for faecal elastase (FE1). If pancreatic enzymes are low they can be replaced using supplements.
Non drug-related causes
If diarrhoea continues for more than a few days, ask for a stool sample to be analysed. Some tests can take a couple of weeks for the results.
Depending on the severity and history of the symptoms and following examination, your doctor may prescribe a course of antibiotics along with anti-diarrhoea drugs to reduce the amount of times you need to go to the toilet.
If lab tests fail to show any bugs, and if symptoms persist, then your doctor may want to perform an endoscopy. This will get a biopsy (a tiny piece of tissue) to be sent for analysis in the laboratory. This can rule out other bowel problems such as colitis. As diarrhoea can be a symptom of other illnesses, it is important to run these tests.
Management and treatment
If nothing shows up in these tests, then the treatment of the symptom itself becomes important.
If you are tolerating your combination generally, you may be able to manage diarrhoea with anti-diarrhoeal drugs or dietary changes, both of which are listed below.
Depending on your treatment options you can also look at changing the drug that is likely to be causing this. Some HIV drugs cause diarrhoea more than others.
Diet
- Drink plenty of fluids to replace the water being lost due to diarrhoea.
- Reducing milk and dairy products in your diet will help if you are lactose intolerant. Alternatives such as rice and soya milk do not contain lactose.
- ‘Rice water’ works as a starch. Boil a small amount of rice in water for 30–45 minutes (or microwave for a shorter time). Flavour with ginger, honey, cinnamon or vanilla when it cools, and then drink during the day.
- Eat less insoluble fibre. Foods that contain insoluble fibre include vegetables, whole wheat breads and cereals, skins, fruit, seeds and nuts.
- Eat more soluble fibre. This is particularly helpful when watery stools are a problem as they help to absorb the excess water and bulk the stool. Soluble fibre is in white rice, pasta. Ispaghula (psyllium) husk (i.e Fybogel or Isogel) and oat bran tablets increase soluble fibre in your diet.
- Reduce caffeine intake as this can can cause the gut to speed up and result in more bowel movements. Caffeine is in coffee, tea and cola. Recreational drugs can have the same effect.
- Eat less high fat and high sugar foods.
- Eat foods rich in potassium such as bananas, peaches, potatoes, fish and chicken. Potassium is lost when you have diarrhoea.
- Try eating live yoghurt to enhance the helpful bacteria in your gut. If you have a problem with dairy products then acidophilus can be taken in pill form. If your CD4 count is under 50 this may not be advisable.
- Whatever changes you make to your diet, make sure it remains balanced. Don’t live on just a few food products, as you will be missing out on essential vitamins and minerals. Ask to see a dietician if you want advice and support about your diet.
Medications and supplements
- Antibiotics are prescribed if a bacterial infection is suspected or detected.
- If pancreatic enzymes are low, supplements like pancrelipase (Creon) or panceatin (Pancrex) can return them to normal levels.
- Fluid and electrolyte replacement (such as dioralyte and sports rehydration solutions like Gatorade etc) are given to rehydrate the body. Recipes are online to make these yourself: ie 1 teaspoon salt, 8 teaspoons sugar, 1 litre of fluid (water, soup, diluted yogurt – but not sugar-based drinks).
- Imodium (loperamide), Lomotil and codeine phosphate are the drugs most commonly prescribed for diarrhoea. They work by slowing gut motions and the speed that you process food, hopefully reducing the number of stools each day. Take with water 30 minutes before food, or as prescribed.
- Your doctor will normally prescribe these first and, for many people, these medications work well. It is important that the medications are taken regularly until the diarrhoea is well controlled. Start with low doses. If the maximum dose (8 pills a day for Imodium) and it is still not controlled, ask your doctor for something else.
- Glutamine has been used experimentally to try and improve bowel function. There is still some debate about the dosage – opinion ranges from 5 g to 40 g a day. It is available either as a powder that must be dissolved in water or a regular pill.
- Bulk forming laxatives are useful when watery stools are a problem. They absorb fluid and bulk out the stool – and lengthen the time the stool stays in the bowel. These drugs are generally taken following a meal and you should not drink for 30 minutes after taking them. Don’t take at the same time as HIV meds. Brands include Fybogel, Isogel, Regulan, Celevac and Normacol.
- Studies on oat bran tablets taken by people with diarrhoea using protease inhibitors were successful and work on the same principle. The dose was 2–3 oat bran tablets before meals or after each protease inhibitor dose.
Treatments:
- Pancreatic enzymes supplements like Creon or Pancrex (if pancreatic insufficiency has been shown)
- Diet changes
- Dioralyte (electrolyte replacement)
- Imodium (loperamide) or Lomotil
- Ispaghula (psyllium husk or seeds)
- Glutamine
- Codeine, tincture of opium or MST (slow-release morphine sulphate)
- Octreotide injections
How opiod anti-diarrhoeals work
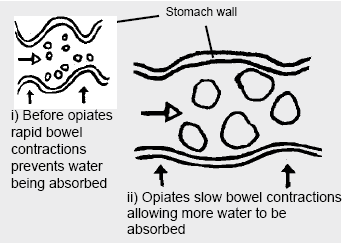
i) Before opiates rapid bowel contractions prevents water being absorbed ii) Opiates slow bowel contractions allowing more water to be absorbed
How bulk-forming agents work

Bulk forming agents contain particles that absorb water and swell up making faeces firmer and more solid
As a last resort…
Slow release morphine sulphate (MST) or octreotide injections can be used if all the usual medications have not worked–although it is used less to control side effects and more to treat other causes of diarrhoea. The slow-release formulation of MST means that low doses of the drug are provided throughout the day. It comes in a wide range of strengths, each coloured differently, so you can be very careful about only taking the dose that you need.
The liquid formulation of morphine sulphate can be used for diarrhoea that occurs at specific times – ie in the hours after dosing.
MST works because one of the side effects of opiates is constipation, and it works by slowing down the gut.
Because it is an opiate, many doctors do not readily offer MST, so you may have to be persistent to get to use it. For some people it is the only thing that works – and even very low doses mean you can return to a normal life.
Last updated: 1 March 2023.
