Fat accumulation
Associated drugs: nukes, NNRTIs, protease inhibitors, possibly integrase inhibitors.
Symptoms
Fat accumulation can occur in the abdomen, breasts, neck and shoulders. It can occur in both men and women. Small bumps or collections of fat, called lipomas, can occur under the skin in other parts of the body including the pubis. A hard fatty lump in a man’s breast is called gynaecomastia.
Abdominal fat can be visceral or subcutaneous. Visceral adipose tissue (VAT) is fat that is around the organs inside the abdomen. Subcutaneous adipose tisue (SAT) is fat under your skin (‘love handles’).
With visceral fat your stomach wall is pushed out from inside. Your stomach muscles can sometimes be quite defined, but your stomach will still be extended.
In severe cases, this can compress your internal organs and interfere with normal functions like breathing and eating.
In these cases there is a greater medical urgency to reverse the fat accumulation. This might help you access treatments like growth hormone releasing factor (GHRF, tesamorelin), growth hormone (rHGH) or to switch to drugs like T-20 or raltegravir.
Treatments for fat accumulation
Many of the approaches used to lower cholesterol and triglycerides are being studied to treat fat accumulation. These also generally include diet and exercise, but also, potentially, new weight loss drugs (ie semaglutide).
Surgery is not usually appropriate for central fat accumulation. However, if appropriate, , liposuction and bariatric surgery are likely to be just as safe and effective for people living with HIV and for the general population. This is based on limited safety studies. Surgery can be used for some localised fat deposits, including breast reduction and for shoulder (dorsocervical) fat.
Using more than one approach might be important. For example, using diet and exercise in addition to anthing else that you try.
Diet means having a healthy balanced diet. It does not mean you should dramtically cut calorie intake, which makes fat loss more difficult.
HIV-related fat accumulation seems to be due to your body signalling itself to produce more fat. Dietary fat is not the only mechanism, but high fat diets are unlikely to help. Low fat diets might help (less and 15% of daily calories from fat). Whatever the cause, diet and exercise seem to be useful in helping reverse these changes.
Anabolic steroids are not recommended for fat accumulation as they are also likely to worsen fat loss.
Metformin can reduce central fat accumulation in people who already have insulin resistance but should not be used if you have a low BMI.
Recombinant human growth hormone (rhGH) can reduce visceral abdominal fat and fat pads from the back of the neck and shoulders. Side effects, including the risk of insulin resistance and diabetes, are reduced using lower doses in more recent studies. Fat accumulation appears to return if rhGH is stopped.
A growth hormone releasing factor called tesamorelin (formerly TH-9507, tradename Egrifta) that can reduce visceral fat by 20% was approved in the US in 2010. It had fewer side effects than rHGH but there is no long-term data (maximum one year).
Tesamorelin is a continual treatment and fat returns if the treatment is stopped. A lower maintenance dose of tesamorelin has not been established.
Neither tesamorelin nor rHGH are approved in Europe as treatments for lipodystrophy. However, rHGH can be prescribed off-label on an individual patient basis. Tesamorelin is unlikely to be approved in Europe in the immediate future as the company withdrew the EU application in June 2012.
Neck, shoulders, breasts and lipomas
Removing fat from the neck or shoulders using liposuction has worked well for some people. The results were sustained in 50% of people but fat returned after several months in 25-50% of people.
There might be a higher likelihood of a permanent result if at the same time, HIV treatment is modified and diet and exercise changed.
Unless the underlying metabolic mechanism is altered, fat accumulation might return after several months.
Liposuction cannot be used for visceral fat accumulation in the abdomen.
Anecdotally, testosterone cream massaged onto the fat pads reduced fat pads on the shoulders. A lower dose should be used for women than for men.
Liposuction and surgery are also used to reduce breast size in both men and women.
Breast lumps (gynaecomastia) in men has been mainly linked to efavirenz, so switching treatment is a first option. However, it is also a common symptom in older men who are overweight. This is because fat can contribute to hormone changes.
If your weight has increased then this could have affected testosterone levels and diet and exercise might help this symptom too.
Some studies reported that low testosterone levels were more linked to larger breast in men than HIV drugs.
Dihydrotestosterone gel (Andractim) might help. Women with lipodystrophy might have higher levels of testosterone than either HIV positive women without lipodystrophy or HIV negative women. It is not clear whether this is due to high insulin levels associated with lipodystrophy, although a link between the length of time on PI-therapy (but not other drugs) and a greater chance of higher testosterone was found in one study.
Talking to your doctor is important as this can be a stressful change in your body. If you are finding this difficult to talk about, take these two studies (both in African men) to show your doctor. Study 1 (Zimbabwe) and Study 2 (Malawi).
Switching HIV drugs
Studies switching individual drugs have been less helpful with fat accumulation than with fat loss. In theory, if one particular drug is linked to these body changes then it is very reasonable to at least try another one, in case this works for you.
If you change your combination, you have to change it to one that is just as effective against HIV.
Switching from efavirenz can reduce breast enlargement in men.
There have been anecdotal reports and case studies of people whose shoulder and/or abdominal fat decreased after switching to atazanavir. A general benefit was not seen in a larger study.
Fat accumulation does not seem closely related to high blood lipids. So far, newer drugs that affect lipids less (unboosted atazanavir, nevirapine, raltegravir and T-20, maraviroc) have not shown reduced rates of fat accumulation.
Figure 4: Illustration of MRI scans
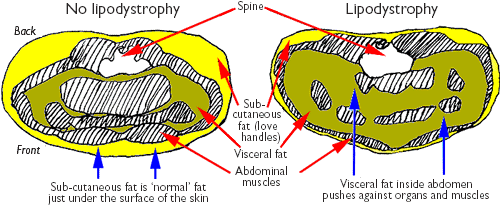
An MRI scan through your stomach shows that fat is inside the abdomen and around the organs rather than being directly under your skin. Key: subcutaneous fat shows as light yellow and visceral fat as olive yellow
Last updated: 1 March 2023.
