Mpox updates: recent publications (2024)
2 February 2024. Related: mpox.
Simon Collins, HIV i-Base
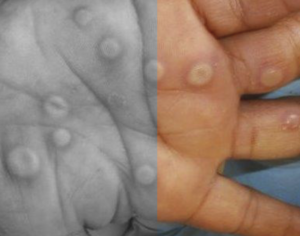 Although the drop in cases in the UK means that mpox is no longer an urgent medical concern, research papers are still being published on important aspects of the 2022 epidemic.
Although the drop in cases in the UK means that mpox is no longer an urgent medical concern, research papers are still being published on important aspects of the 2022 epidemic.
This page will signpost to interesting papers as they become available in 2024.
Eight papers were also reviewed in December 2023. [1]
Tissue biopsy results from severe mpox cases
An analysis of biopsy and autopsy tissues from 22 people in the US with severe or fatal outcomes from mpox that characterised the pathology and viral antigen and DNA distribution. Testing for coinfections was also performed. 20/22 were living with HIV, all with a CD4 count <159 cells/mm3 (14/29 with a count <50 cells/mm3) and two lung transplant recipients on immunosuppresive medication.
Severe mpox was characterised by extensive viral infection of tissues and viraemic dissemination that progressed despite available treatment. Digestive tract and lung involvement are common and associated with prominent histopathological and clinical manifestations. Coinfections may complicate mpox diagnosis and treatment. [2]
Mpox reinfections and breakthrough infections after vaccines
A global case series of eight hMPXV reinfections and 30 vaccine breakthrough infections together with an editprial comment. [3, 4]
The findings confirm that neither natural immunity from a previous infection nor immunity conferred by vaccination offer complete protection against hMPXV reinfection or infection. However previous immunity did appear beneficial in terms of disease severity: repeat infections or infections after vaccination were characterised by fewer lesions and a faster resolution of disease leading to a decreased Mpox Severity Score System score. [3]
Behavioural change reduced UK mpox outbreak: vaccination essential to reduce future risks
Behaviour change is credited with having a key role in reducing new infections during 2022. [5]
Mpox as AIDS-defining event
A 59-year-old man with previously undiagnosed HIV presented with a severe and protracted course of mpox that did not respond to mpox treatment. Advanced HIV included a CD4 count of 27 cells/mm3, CD4% of 2.4 and viral load >520,000 copies/mL. [6]
The most recent negative HIV tests was seven years earlier. This person worsened clinically with new mucocutaneous lesions and necrotic evolution of pre-existing ones. Mpox viral shedding persisted for 11 months.
ART was only started 10 days after the HIV diagnosis and tecovirimat 20 days after presentation. Skin lesions didn’t start to resolve until five months when they were able to be discharged home, with CD4 count at 75 cells/mmm3.
They were diagnosed with COVID-19, ten days later. Although the case notes comment on this person having received a full vaccinations, there is no awareness that the these are unlikely to have produced a vaccine response give the very low CD4 count.
This case highlights the importance of routine HIV testing to minimise the risk for mpox-, COVID- and HIV-related serious events.
Tecovirimat and mpox treatment
Results from a prospective cohort study provide new data supporting the early use of tecovirimat within seven days of mpox symptoms. The study included people living with HIV who were diagnosed with mpox between June amd October 2022 at four HIV clinics in Atlanta, Mpox disease progression occurred in 3 (5.4%) vs 15 (26.8%) individuals in the early vs late/no groups respectively. This represented an odds ratio for progression of 11.0 (95% CI: 1.4 to 85.1), p=0.002 with late/no vs early tecovirimat. The median time to symptom progressions was also significantly longer for those using early tecovirimat: median 22 days (IQR: 4 to 57) vs 4 days (IQR: 2 to 12), respectively. [7]
An editorial comment on the above study suggested caution before universally prescribing tecovirimat to everyone with mpox, especially given the limitations of observational data and limited access to tecovirimat. The potential for confounding and the wide confidence interval for the primary endpoint was also noted. [8]
A recent paper in PLoS usefully reviews some of the difficulties faced by international tecovirimat studies. This includes the lack of a fast-track approval process, apparently learning little from the experiences of COVID-19. It also highlights how the drive for research is still closely tied to potential commercial outcomes in high-income countries. [9]
References
- Mpox update: recent publications (2023). HTB December 2023.
https://i-base.info/htb/46896 - Ritter JM et al. Pathology and monkeypox virus localization in tissues from immunocompromised patients with severe or fatal mpox. The Journal of Infectious Diseases, 2024; jiad574. (18 January 2024).
https://doi.org/10.1093/infdis/jiad574 - Hazra A et al. Mpox in people with past infection or a complete vaccination course: a global case series. Lancet Inf Dis 24(1)57-64. (January 2023).
https://doi.org/10.1016/S1473-3099(23)00492-9 -
Shamier MC et al. The implications of mpox breakthrough infections on future vaccination strategies. Lancet Inf Dis. Comment. 24(1):6–8. (January 2024).
-
Shen M et al. Targeted interventions for individuals at high risk is essential for mpox control. Lancet Inf Dis. 24(1);8-9. (January 2024)
-
Pinnett C et al. Mpox as AIDS-defining event with a severe and protracted course: clinical immunological and virological implications. Lancet Inf Dis, 24(2);E127-E135. (February 2024).
https://doi.org/10.1016/S1473-3099(23)00482-6 - Early Tecovirimat Treatment for Mpox Disease Among People With HIV. JAMA Internal Medicine Research. (8 January 2024).
https://jamanetwork.com/journals/jamainternalmedicine/article-abstract/2813862 - Tecovirimat for Mpox—Promise and Limitation. JAMA Internal Medicine. Opinion. (8 January 2024).
https://jamanetwork.com/journals/jamainternalmedicine/article-abstract/2813863 - Olliaro P et al. (2024) Mpox: The alarm went off. Have we gone back to sleep? PLoS Negl Trop Dis 18(1): e0011871.
https://doi.org/10.1371/journal.pntd.0011871

