Viral load

Viral load is the most important factor in the risk of HIV.
U=U means that HIV cannot be transmitted if viral load is undetectable.
So viral load is more important than condom use.
Viral load determines how infectious bodily fluids are. Levels are highest in someone who is recently infected (up to 40 million copies in a millilitre of blood). By comparison, someone on treatment with an undetectable viral load has less than 50 copies/mL (see Figures 2 and 3). [3]
When viral load is very high, low risk activities like giving oral sex become a higher risk.
If viral load is undetectable, there is zero risk of HIV.
PrEP also protects against HIV, even when viral load is very high.
in 2014, the PARTNER study reported no linked HIV transmissions when viral load was undetectable.
This was in 900 couples who had sex more than 58,000 times without using condoms. [1]
Importantly, this study included gay couples and anal sex (gay and straight).
It included periods when viral load was likely to blip between tests and when there were other STIs.
In 2018, the PARTNER 2 study produced even more evidence to support the safety in gay men. This time, with no transmissions after couples had sex 77,000 times without condoms. [2, 3]
This article includes the evidence for U=U: that undetectable viral load makes HIV untransmittable.
https://i-base.info/htb/32308
Figure 2 – Viral load levels as HIV infection progresses
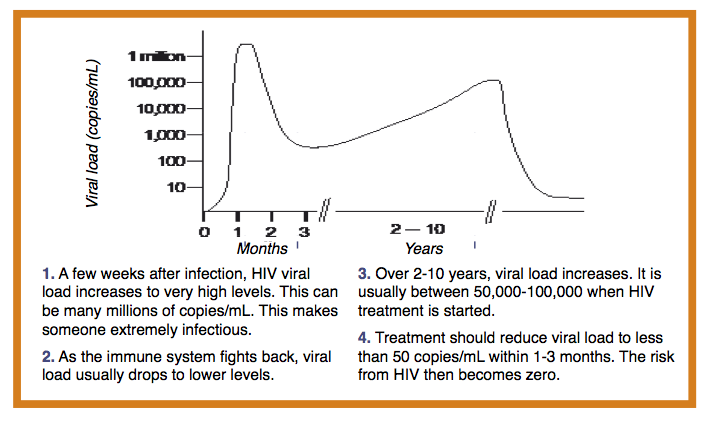
Figure 3 – The relationship between viral load and HIV transmission in Rakai Study [4]
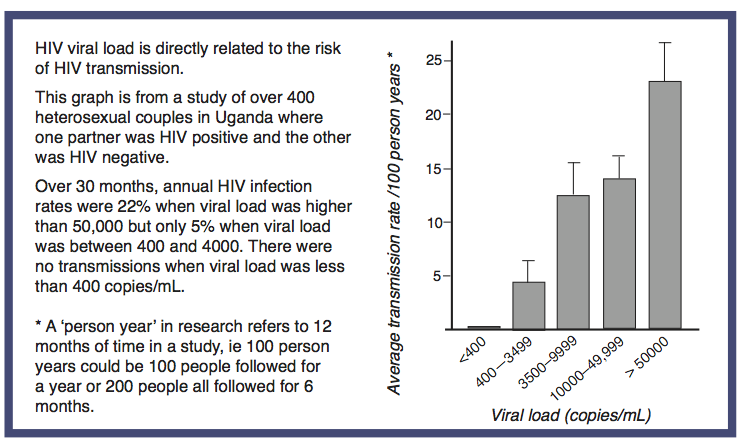
NOTE: Person years is used when calculating risks. It allows for all the time that different people contribute to a study, even when this might be years for one person and only months for another.
References
- Rodger AJ et al for the PARTNER study group. Sexual activity without condoms and risk of HIV transmission in serodifferent couples when the HIV-positive partner is using suppressive antiretroviral therapy. JAMA, 2016: 316(2):1-11. (Free online).
http://jama.jamanetwork.com/article.aspx?articleid=2533066 - Rodger AJ et al. Risk of HIV transmission through condomless sex in serodifferent gay couples with the HIV-positive partner taking suppressive antiretroviral therapy (PARTNER): final results of a multicentre, prospective, observational study. Lancet 2019; published online May 2. (Open access). DOI: 10.1016/S0140-6736(19)30418-0
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(19)30418-0/fulltext - Zero HIV transmissions in PARTNER study after gay couples had sex 77,000 times without condoms – an undetectable viral load stops HIV. HTB July 2018.
https://i-base.info/htb/34604 - Quinn TC and others. Viral load and heterosexual transmission of HIV type 1. Rakai Project Study Group. New England Journal of Medicine 2000; 342: 921-929.
http://www.nejm.org/doi/full/10.1056/NEJM200003303421303
Last updated: 1 June 2024.
