The HIV lifecycle in detail
Like other living things, viruses need to be able to reproduce.
When viruses reproduce it is called replication. HIV uses CD4 immune cells to replicate. And each infected CD4 cell produces hundreds of new copies of new HIV particles.
The process is called the HIV lifecycle.
Each replication cycle only lasts 1 to 2 days. It has several stages and different HIV drugs are active at different stages. HIV drugs are called inhibitors because they inhibit or stop parts of the cycle.
- HIV first has to attach to a CD4 cell. The proteins on the outer surface of HIV (called gp41 and gp120) connect with receptors on the surface of the CD4 cell (usually the CD4 receptor and the CCR5 coreceptor).
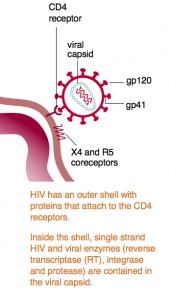
- HIV drugs that block this process are called entry inhibitors. This family of drugs block attachment to gp41 or gp120 on the CD4 receptor or block the coreceptor CCR5. Monoclonal antibodies (mAbs) can also block this stage.
- After HIV attaches to the CD4 cell, the capsid is released into the main body of the cell (called the cytoplasm). The capsid then enters the cell nucleus and releases three key enzymes. These are the proteins that HIV uses to replicate.
- These enzymes then work in the nucleus. The first enzyme is called RT. This stands for reverse transcriptase. RT changes the single strand of HIV (called RNA) into a double strand to fit in with human DNA. Two different types of RT inhibitors (RTIs) block this process: (i) nucleoside/tide (NRTIs/NtRTIs), and (ii) non-nucleoside (NNRTIs).
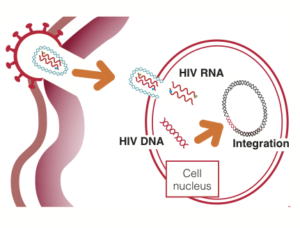
- The new double-stranded HIV can now be integrated into human DNA. Drugs that block this process are called integrase inhibitors, abbreviated to INSTIs.
- The CD4 nucleus then starts producing raw material to make new HIV. These long strands of new HIV particles need to be cut up and assembled as new virus. The enzyme involved in the cutting and assembling process is called protease. The HIV meds that block this process are called protease inhibitors.
- The newly formed virus then has to leave the cell. Although there are currently no HIV drugs that block this stage, several drugs are in development. Budding inhibitors stop new HIV from leaving of the CD4 cell. Maturation inhibitors block the final assembly process.
- The newly released viruses (called virions) go on to infect new CD4 cells – to repeat the process over again. The old CD4 cell then dies. This continuous process happens millions of times every day when not on ART. Without ART, HIV is one of the most active and rapidly reproducing virus.
An important concept about ART, is that HIV drugs only work on CD4 cells in your body that are awake and actively producing HIV.
However, most CD4 cells in your immune system are sleeping or resting. The resting cells, even if they contain HIV, are not affected by ART.
Reaching HIV in resting cells is a main aim in HIV cure research.
Key points
- HIV uses CD4 cells to replicate.
- Different HIV medications block different stages of the HIV lifecycle.
- Each infected CD4 cell produces about 300 new infectious
viruses – called virions. - ART stops the HIV lifecycle. On ART, the only virus in your body is in sleeping or resting CD4 cells.
- You need to continue taking ART every day because some of these sleeping cells wake up every day.
Main types of HIV drugs
There are six main types (or classes) of drugs that work against different parts of the HIV lifecycle.
There are more than 30 HIV drugs and formulations. Only a few combinations are now commonly used.
| Abbreviation | Full names | |
| NRTIs/NtRTIs (nukes) | Nucleoside/tide reverse transcriptase inhibitors or nucleoside/tide analogues. | |
| NNRTIs (non-nukes) | Non-nucleoside reverse transcriptase inhibitors. | |
| PIs | Protease inhibitors. | |
| INIs (or INSTIs) | Integrase (strand transfer) inhibitors. | |
| CCR5 inhibitors | CCR5 inhibitors are a type of entry inhibitor. | |
| Fusion inhibitors | Fusion inhibitors are a type of entry inhibitor. | |
| mAbs or bNAbs | Monoclonal antibodies block HIV entering the T-cell. | |
| CIs | Capsid inhibitors. |
Last updated: 1 January 2025.
