GLP-1 receptor agonists reduce substance use disorder: a role for addiction to chemsex drugs?
6 March 2026. Related: Special reports, Side effects, Coinfections and complications.
Simon Collins, HIV i-Base
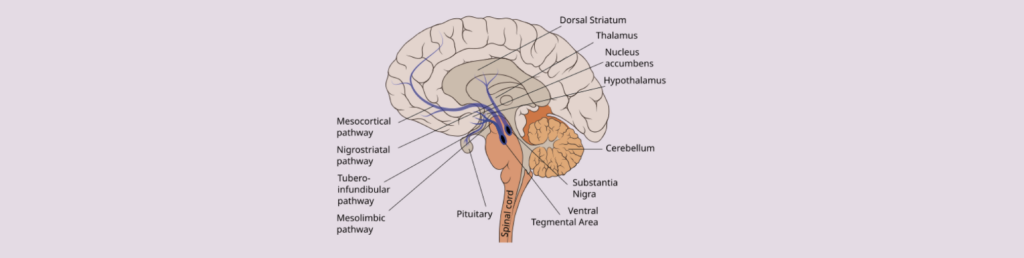
When i-Base reported several GLP-1 studies in people living with HIV from CROI 2024, we included a discussion about whether anecdotal reports of breaking the dopamine reward pathway associated with reduced craving for food might help reduce dependence on chemsex drugs which currently have no effective treatment to support and manage withdrawal. [1]
Breaking the craving for food is a potential mechanism for the dramatic weight loss seen with GLP-1 receptor agonist (RA) – and anecdotal reports about people on treatment drinking less alcohol and smoking fewer cigarettes has also been reported in a small phase 2 study. [2]
Mixed results have been reported though in several other studies.
A new paper in the BMJ from a large observational database study now adds substantial data to this potential benefit for use in substance use disorder (SUD). [3]
This study involved more than 680,000 veterans with diabetes (mean age 65 years, 90% male, 80% white) who received their care in the large US Department of Veterans Affairs healthcare programme and who were treated with GLP-1 receptor agonists in two protocols. Protocol 1 compared use of GLP-1 receptor agonists to SGLT-2 inhibitors in ~600,000 people without SUD at baseline in separate emulated studies for each substance. Protocol 2 was a single study in ~81,000 people with existing SUD who used GLP-1 receptor agonists or SGLT-2 inhibitors. GLP-1 RAs were used by approximately 25% of participants in each study.
The results showed a clear and consistent reduction in the use of cannabis, cocaine, nicotine, opioid and other substances, together with reduced hospital visits, mortality and suicide. See Table 1.
The use of GLP-1 receptor agonists compared to SGLT-2 inhibitors was associated with significantly reduced risk of disorders related to each substance in Protocol 1 and significantly fewer clinical events in Protocol 2.
Median follow-up was 3 years (IQR: 2.26 to 3.00), with more than 1,353,000 person-years of follow up. Adherence analyses also supported the direction of this effect.
Table 1: Different risk of incident substance use disorders and clinical events
| Substance / event | HR | 95%CI | NRD per 1000 people (95%CI) |
| Protocol 1: Incident SUDs by substance (n=606,434) | |||
| Alcohol use | 0.82 | 0.78 to 0.85 | −5.57 (−6.61 to −4.53) |
| Cannabis use | 0.86 | 0.81 to 0.90 | −2.25 (−3.00 to −1.50) |
| Cocaine use | 0.80 | 0.72 to 0.88 | −0.97 (−1.37 to −0.57) |
| Nicotine use | 0.80 | 0.74 to 0.87 | −1.64 (−2.19 to −1.09) |
| Opioid use | 0.75 | 0.67 to 0.85 | −0.86 (−1.19 to −0.52) |
| Other SUDs | 0.87 | 0.81 to 0.94 | −1.12 (−1.68 to −0.55) |
| Composite of all incident SUDs | 0.86 | 0.83 to 0.88 | −6.61 (−7.95 to −5.26) |
| Protocol 2 (SUD-related clinical events) (n=81, 617) | |||
| ER visits | 0.69 | 0.61 to 0.78 | −8.92 (−11.59 to −6.25) |
| Hospital admissions | 0.74 | 0.65 to 0.85 | −6.23 (−8.73 to −3.74) |
| Mortality | 0.50 | 0.32 to 0.79 | −1.52 (−2.32 to −0.72) |
| Drug overdose | 0.61 | 0.42 to 0.88 | −1.49 (−2.43 to −0.55) |
| Suicidal ideation or attempt | 0.75 | 0.67 to 0.83 | −9.95 (−13.14 to −6.77) |
Key: HR = Hazard ratio, CI = Confidence Interval, NRD = net 3-year risk difference per 1000 people
An accompanying editorial stressed the impact on reducing risk in people with existing SUD. [4]
Also important, is how few people are able to maintain GLP-1 RA treatment. A large retrospective US insurance database study (40 million people) looked at persistence of treatment for more than a year and adherence amongst almost 127,000 people without diabetes who were prescribed a GLP-1 RA between 2019 and 2024. [5]
Mean age was 45 (SD +/– 10 years), 80% were women, and optimal adherence was defined as >80% doses without more than a 60-day period without treatment. Switching between GLP-1 RAs was allowed and was common (approx 20%), perhaps reflecting active management.
Results included that only about 50% were categorised as having optimal adherence and that less than 1 in 4 were still taking these drugs after 12 months.
comment
These data support pilot studies to see whether GLP-1 agonists could have a similar protective role in other substance use disorders that affect people living with HIV and other marginalised communities.
This includes to break the use and need for chemsex drugs that include methamphetamine (crystal/crystal meth/Tina/meth), mephedrone (meph) and GHB/GBL (G, Gina).
Although the manufacturers of these drugs have not supported research studies that include people living with HIV, it might become possible to plan new research now in countries where patents on semaglutide expire in 2027.
Please see the open-access paper for full details.
References
- CROI 2024: HIV studies with semaglutide: significant benefits but limited access for treatment and research. HTB (10 March 2024).
https://i-base.info/htb/47286 - Semaglutide reduces alcohol and cigarette use in a randomised phase 2 study. HTB (12 February 2025).
https://i-base.info/htb/50245 - Cai M et al. Glucagon-like peptide-1 receptor agonists and risk of substance use disorders among US veterans with type 2 diabetes: cohort study. BMJ 2026392:e086886, doi: 10.1136/bmj-2025-086886 (04 March 2026).
https://www.bmj.com/content/392/bmj-2025-086886 - Fares Qeadan. Metabolic medicines and addiction: what GLP-1 receptor agonists might add to substance use care
BMJ 2026;392:s325. (04 March 2026).
https://www.bmj.com/content/392/bmj.s325 - Xie L et al. Glucagon-Like Peptide-1 Receptor Agonist Switching and Treatment Persistencein Adults Without Diabetes. JAMA Network Open. 2026 9(3):e261272. doi:10.1001/jamanetworkopen.2026.1272. (10 March 2026).

