England’s HIV Action Plan: on-target for HIV 2030 goals on preventable deaths but not for diagnoses: key populations still not included
14 May 2026. Related: Special reports, Treatment strategies, HIV prevention and transmission.
Simon Collins, HIV i-Base
On 14 May 2026, an impressive 48-page monitoring and evaluation report was published by UKHSA, detailing progress towards HIV health targets for 2030. [1]
These include reducing HIV diagnoses and HIV-related preventable mortality by 90% compared to 2010 figures – and sustainability plans for after 2030. [2]
However, most UNAIDS key populations are still not included.
Introduction and summary
The new report uses data from England in 2024 on the numbers of people living with HIV, accessing ART, disconnected from care and recent diagnoses, with breakdowns by demographics that include age, sex, ethnicity, HIV risk and geographical region.
In 2024, England reported UNAIDS-defined 95:95:95 targets as 95% 94% 98% (for those diagnosed, on ART and with undetectable viral load, respectively). However, using two new upper- and lower-estimates models, England would qualify these as 95:95:96 and 95:94:91, respectively.
In summary, reducing new diagnoses to only of 532 by 2030 is not currently on track or achievable. However, the goal of reducing HIV-related deaths to only 27 by 2030 is reported as being both on-track and included as achievable, although based on limited data. See Table 1.
Table 1: Progress in England towards 2030 targets
| Target | 2010 actual | 2024 target | 2024 actual | 2030 target | comment |
| New diagnoses | 5321 | 1969 | 2773 | 532 | Not currently on track or achievable either overall or for most demographics. (see Figure 1). |
| Preventable HIV-related deaths* | 267 | 99 | 90 | 27 | Ahead of target and achievable. |
* HIV-related deaths are defined as when HIV is a contributing factor, including for virally mediated cancers and side-effects from ART. However, preventable deaths are defined in relation accessing appropriate care, often due to late or missed diagnoses, or detectable viral load on ART. [4]
Key data points for England based on 2024 data
The following summary points were included in the report.
- 114,000 adults (age 15 or older) are estimated to be living with HIV .
- Of these, 6,000 people (just over 1 in 20) are not yet diagnosed.
- 102,100 adults were on ART (95%), of whom, 99,600 were undetectable (98%).
- At least 14,300 people (1 in 10) have detectable viral load (but possibly up to 21,500). This includes 6000 people who are undiagnosed, 5,800 who are diagnosed but not on ART and 2500 with detectable viral load (>200 c/mL) on ART.
- More than 5% of people diagnosed with HIV are no longer accessing care which is important as UNAIDS targets only related to those in care. By demographics, this included more than 1,500 white gay and bisexual men more than 770 Black African heterosexual women.
- There were 2,773 new HIV diagnoses in England in 2024.
- Of these, 928 people were diagnosed late (42%, although this is based on a lower denominator of only 2,196 diagnoses due to missing CD4 data). Numbers and proportions differ by sexuality and ethnicity, ranging from 27% of ethnic minority gay and bisexual men to roughly 56% of African heterosexual men.
- Of late diagnoses, 539 (25% based on the 2,196 denominator) were categorised as very late defined as having a CD4 count <200 cells/uL.
- Roughly 90 of the 643 deaths were defined as being due to preventable HIV-related causes, including late diagnosis. These figures are complicated by limited and missing data.
- 111,000 people accessed PrEP (80% of gay and bisexual men who could benefit vs roughly 35% in Black African heterosexuals.
- A higher percentage of positive tests are now reported in primary and secondary care and community settings than in sexual health clinics. Also, roughly 4% of new diagnoses were from partner notification.
- Roughly 6-7% of people reported HIV-related stigma when accessing care.
Progress towards 2030 targets
Figures 1 and 2 summarise recent trends in both HIV diagnoses and preventable mortality, and show the 2030 goals.
Maintaining these rates of change however, might not be linear due to complicated factors associated with each goal.
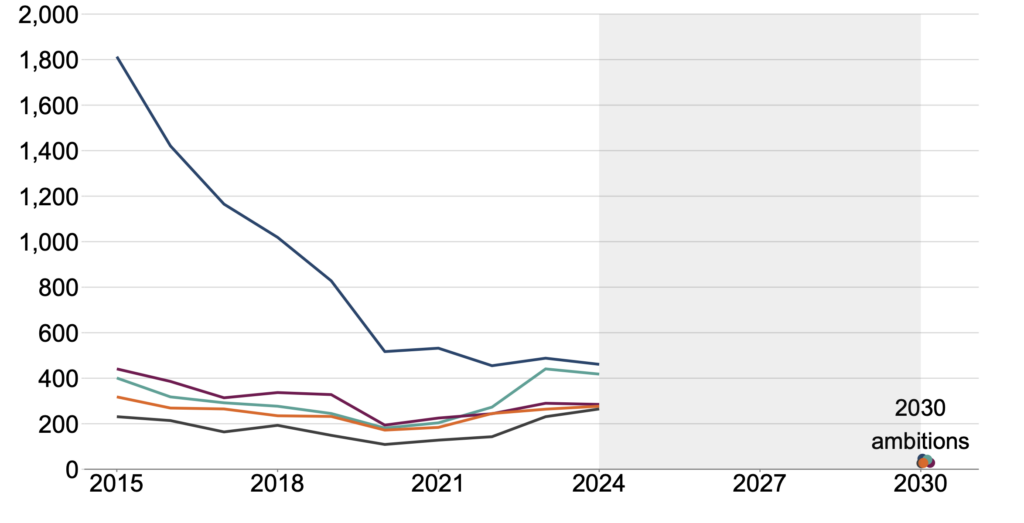
Figure 1: Recent trends in HIV diagnoses
Key (top to bottom): White gay and bisexual men; Black African heterosexual women; ethnic minority gay and bisexual men; other ethnic minority heterosexuals; Black African heterosexual men.
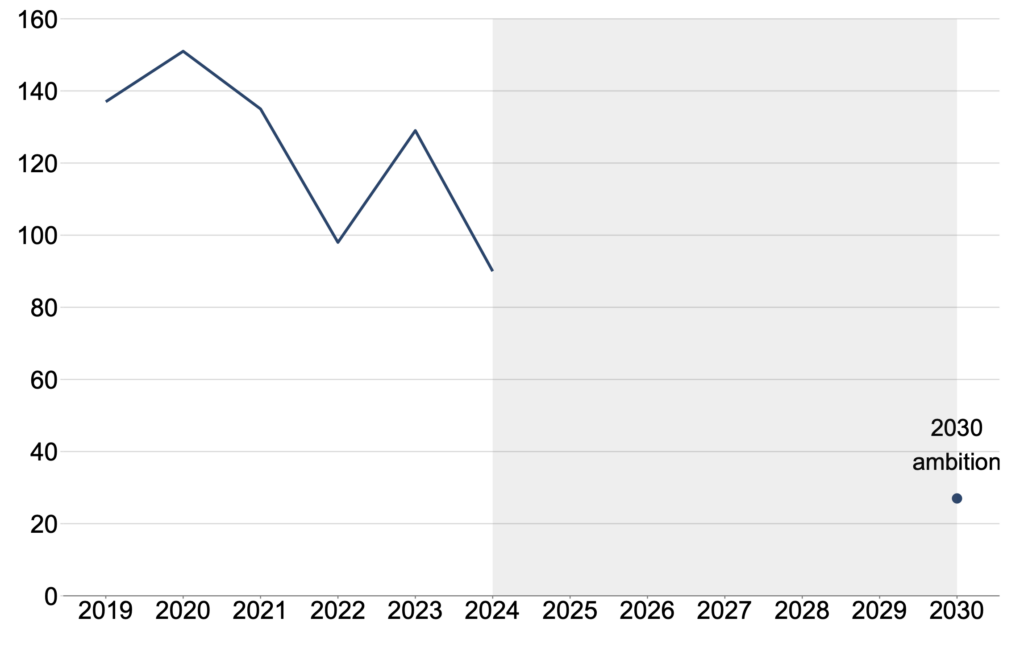
Figure 2: Recent trends in preventable HIV related mortality
Main challenges and priorities
The main challenges in the report include:
- Overcoming current inequity to PrEP access including by ethnicity and sexuality.
- Expanding access to HIV testing outside of sexual health clinics, including in primary care.
- Investing in new initiative to support re-engagement in care.
- Dveloping HIV sensitivity training for health workers training that also includes equality and diversity.
The report also includes five main priorities with appropriate indicators.
- HIV prevention largely based on more expanding more equitable access to PrEP.
- Expanding new models and venues for HIV testing, including in community settings, to reduce ongoing transmissions and late diagnoses.
- To rapidly link people to care with access to effective ART and to effectively reengage people in care.
- To reduce stigma and increase quality of life for people living with HIV. However, the only marker for this goal will be results from the next Positive Voices survey and the only action to contribute to change, is to develop training for health workers.
- To strengthen the overall healthcare system to improve HIV-related services, including for HIV drug resistance, retaining health workers, increasing network visibility,
comment
This report is welcomed and shows the continued commitment to achieving ambitious goals for HIV in England by 2030.
This will involve new strategies to achieve equity of access to prevention and testing services, especially for Black African heterosexuals. It will also include new pathways that take options for PrEP and HIV testing to primary, secondary and community settings, while still maintaining services at sexual health clinics.
Achieving the goals will also depend on whether there is a continued linear relationship for each target and that this continues to zero.
Also, despite these exciting plans, it is disappointing that several community concerns in the original HIV Action Plan are still not addressed.
For example, other than gay and bisexual men, there are no references to the other four UNAIDS key populations, none of who are even mentioned:
- Sex workers
- People who inject drugs
- Transgender people
- People in prison (and detention centres).
Please see the full report for more details.
References
- gov.uk. HIV Action Plan Monitoring and Evaluation Framework report 2026. (14 May 2026).
https://www.gov.uk/government/publications/hiv-action-plan-monitoring-and-evaluation-framework/hiv-action-plan-monitoring-and-evaluation-framework-2026-report - gov.uk. HIV Gov.uk. HIV Action Plan for England 2025 to 2030. (1 December 2025).
https://www.gov.uk/government/publications/hiv-action-plan-for-england-2025-to-2030/hiv-action-plan-for-england-2025-to-2030 - HIV Action Plan for England: £170m to reduce new diagnoses and re-engage people in care – but are targets achievable? HTB (1 December 2025).
https://i-base.info/htb/52901 - Croxford SE et al. Recommendations for defining preventable HIV-related mortality for public health monitoring in the era of Getting to Zero: an expert consensus. Position paper. Lancet HIV (10)3; E195-E201. DOI: 10.1016/S2352-3018(22)00363-0. (4 January 2023).
https://www.thelancet.com/journals/lanhiv/article/PIIS2352-3018(22)00363-0/fulltext