Meeting calls for NHS funding and training to provide repair treatment for people with facial lipoatrophy
10 March 2002. Related: Special reports, Treatment access, Side effects, Weight, diabetes, metabolic complications.
Graham McKerrow, HIV i-Base
A meeting of more than a 100 doctors, nurses and patients at the Royal Society of Medicine in London, heard repeated calls for the National Health Service to offer New-Fill treatment to people with facial lipoatrophy (fat loss).
Speakers called for advice on the use of New-Fill to be included in the official guidelines on treating HIV, for political pressure to be exerted on the NHS to pay for this treatment, and for the establishment of a contact forum where people who are considering the treatment would be able to talk to those who have had it.
The meeting, organised by HIV i-Base, publishers of this journal, and the Royal Free Hospital in London, heard from people who said lipoatrophy had caused them a range of social and psychological problems. One man said he had been turned down for jobs because of it, and a woman spoke about spending a morning weeping in front of a mirror.
Patients and medical professionals were united in calling for the health service to provide treatment. All the HIV commissioners for the London health authorities – the NHS managers who decide what the health budget will be spent on – were invited to the meeting, on 24 January, but none attended. One man with lipoatrophy told the morning session: “I am very disappointed the commissioners aren’t here today; I’m very angry they aren’t here today.” However, there was a round of applause for the presence of Barbara Disney who works for the London Borough of Camden and is a senior development officer representing the local authorities on the London Health Authorities Commissioning Group.
Speakers urged patients and professionals to lobby the commissioners to pay for the treatment – which consists of injecting New-Fill – a hydrogel of Polylactic Acid (PLA) – into the face to improve facial appearance of people who have lost fat. People were encouraged to lobby their MPs to put pressure on the commissioners. Some speakers called on the British HIV Association (BHIVA) to lead the way. Dr Mike Youle of the Royal Free Hospital, London, said: “What we need to do is unlock the money and train the people to do it.” A man from Liverpool said the cost of PLA should be included in the budget for HIV care.
Several people spoke about being treated by Harley Street doctors where the treatment costs £400 to £500 a session and commonly requires three to six sessions.
The meeting heard reports from around the country of what is happening in the NHS; several hospitals are running trials while some are siphoning money from other budgets to treat a small number of people. Speakers included doctors from Paris who have extensive experience of treating people with PLA and a plastic surgeon from New York who outlined other options, particularly transplanting fat from other parts of the body.
French patient survey reveals demand for PLA and need for information
Emmanuel Trenado of the organisation AIDES in Paris outlined the results of a patient survey he carried out in France at the end of last year, in which 248 patient-completed questionnaires were analysed to evaluate the need for and the obstacles to treatment, and to collect reports of patient satisfaction with treatment.
Of those surveyed, 84.7% were men; most were aged between 30 and 49 years and had been positive for more than 10 years. More than 67% had been on antiretroviral therapy for more than five years. They suffered from prominent veins and loss of body fat and buttocks. Almost one in four, 23% said they could not discuss the problem with their doctors. Only 23.4% said they had access to ‘repair procedures’.
Of those who had been treated, 67.9% had been given filling products such as PLA, and 91.1% of them were treated in 2000 or 2001. Nearly three out of four, 72.5% were given PLA, and 12.5% were given Hyaluronic Acid (Restilane and Perlane, for example). Most (51%) of those who had been treated with filling products had three to five injections. Only 9.8% required more than five injections.
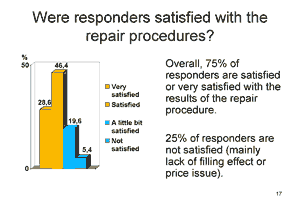
The overwhelming majority, 86.8% said they tolerated the procedure ‘well’ or ‘very well’. Seventy five per cent of responders were ‘satisfied’ or ‘very satisfied’ with the results of the repair procedure and 5.4% said they were not satisfied, mainly because of insubstantial filling effect or the cost. Of those who did not access treatment, 50.8% said it was because of a lack of information and 39.6% said it was because of the cost. Most, 86.9%, said they wanted access to the treatments. Almost 80% wanted filling products rather than surgery or other types of treatment.
Trenado concluded that the vast majority did not have, but wanted, access to repair procedures. Filling products were the repair procedure most commonly used. The responders who had undergone the repair procedures were pleased with the results. The study found a need to better inform people about facial lipoatrophy, and a need to address the question of how treatment would be paid for.
Mike Youle, who was chairing the meeting, pointed out that treatment in the UK was approved on an individual hospital basis, and its availability depended on how much people lobbied for a particular treatment, whereas France has a much more even provision across the country.
Limited availability of PLA in the UK
Some hospitals in the UK are already offering treatment to a few patients and it was stressed that when available this was only to existing patients. Doctors reported the following pattern of provision:
University College Hospital, London. Dr Ian Williams said the Mortimer Market Centre was working with colleagues in plastic surgery and hoped to provide PLA and collagen. They are seeking funding for this.
North Manchester General Hospital. Dr Ed Wilkins said they had set up a study, and 33 patients had received injections of PLA. He was trained in the procedure by Dr Elizabeth Laglenne from Paris, who also spoke at the meeting. He said it was a relatively simple procedure to learn and administer, although there was some debate among the medical professionals at the morning session about whether it should be carried out by HIV doctors, nurses or plastic surgeons. The Manchester study is looking at the quality of life implications of treatment, as well as measuring the physical results by scanning the thickness of the skin before and after treatment. He said that so far 75% show a good improvement and 25% a very good improvement. They have applied for funding.
St Mary’s Hospital, London. Dr George Scullard said they were working with dermatologists and were about to treat between 20 and 30 people.
Chelsea and Westminster Hospital, London. Charge Nurse Sharon Brown reported that many more people required the treatment than could be found places on the pilot scheme they are running.
East London. Dr Tom McManus of Newham General and the Royal London, said they were investigating fat transfer work with the New York plastic surgeon Dr Jeff Brande, but there was “no interest” from the local NHS commissioners.
King’s College Hospital, London. Dr Chris Taylor said they were exploring ways of funding treatment.
Royal Free Hospital, London. Dr Youle said they had approached a plastic surgeon colleague and had been planning to work together but the plastic surgeon has moved to another job. They would take the matter up with the new plastic surgeon, and Dr Youle said: “I think this will be in our next year’s budget.”
Ealing Hospital. Dr Stephen Ash said he had treated 12 people with PLA, and added: “So far the patients are very happy with the outcome.” The treatment has been paid for by taking money from another budget. Dr Ash added: “It would help if it was in the BHIVA guidelines.”
The doctors emphasised that treatment was only available for a limited number of registered patients, and that this treatment would not be available to new patients who were switching treatment centres solely to access New-Fill.
People with facial wasting tell of trauma, and the need for repair treatment
A substantial part of the meeting was devoted to discussion by patients about the consequences of having facial lipoatrophy and the experiences of those who had received repair treatment. Bryan Thompson said: “It was literally a three month period where my face just began to fall off. The thing about facial lipoatrophy is that it blows your cover; people realise. Every day it was there and a constant reminder that I was HIV positive.
Kate Thomson, told the meeting about being in tears over the way she looked and the lack of information about treatment: “I looked like I had aged about 20 years in a matter of months. Today is the first time I have met anyone who has had the procedure and we need to get the information out there so that people can access it.” She said she had had to deal with advice from people who thought she was anorexic.
One man, an actor by profession, had a course of three injections at the Chelsea and Westminster Hospital “and I can’t wait for the fourth one.” When he developed lipoatrophy, he was shocked by his facial appearance, and “devastated” when he saw his mother’s reaction. Lipoatrophy had cost him work; at one point his agent said to him: “There is no way you can do anything with a face like that.” He said: “I am really grateful I got onto the [PLA] trial. I think it should be available for everybody because it does make a huge difference.”
French doctors outline the advantages of PLA
Dr Elizabeth Laglenne of Paris, who has worked for 20 years with silicone and other implants made one of the most impressive contributions to the meeting. Seven years ago she learnt about PLA and started using it. She said there is more information on it than some people think; there have been studies conducted in the Netherlands, Belgium and other countries, as well as in France.
Fillers like PLA and collagen are good for people who don’t have any fat to transplant, she said. Collagen requires a lot of injections and is more expensive than fat transplants or PLA “and it is too difficult”. She said: “New-Fill has been on the market for a few years and we have followed it for three years after treatment.”
Dr Laglenne said: “If you have money, you can pay for treatment but we must do something for the most important population: people without money.” As well as seeing private patients, she has also treated 500 people without charge, such is the demand. She said the treatment is getting better as techniques are improved; for example they now slightly dilute the product to make the injections easier and to give a smoother result. Some people have complained that the injections hurt, but this can be relieved by first applying an anaesthetic cream to the skin and also including an anaesthetic mixed into the product.
Also from Paris was Dr Camille Aubron-Olivier of the Hôpital Pitié-Salpêtriére, who reported on the Vega study of the safety and efficacy of PLA treatment in positive people with severe facial wasting. It is an open label, two centre, pilot study, which started in May 2000 and is following 50 patients for 24 months. Patients attending the Hôpital Pitié-Salpêtriére and the Royal Free Hospital in London were given three sets of injections, each of 3ml of PLA, 15 days apart and, for those who needed it, a fourth set of injections. Each set of injections involves 20-40 small injections into each cheek. All have been on antiretroviral therapy for more than three months, on HAART for less than three years, have plasma HIV viral load <5000 copies/mL for at least three months, and subcutaneous adipose tissue of the cheek measured by ecography <2mm.
The subjects are photographed, inspected, and their skin thickness is measured after six months, 12 months, 18 months and 24 months. Evaluation looks at quality of life as well as blood counts and changes in antiretroviral medication.
The preliminary results show no serious adverse events and measurable thickening of treated skin. Dr Aubron-Olivier said: “The high degree of satisfaction of all our patients is surely the most important result of our study.”
Research now underway in London
Sharon Brown from the Chelsea and Westminster Hospital, London, spoke about the randomised, open label study of PLA injections for buccal (cheek) fat pad wasting in people with HIV-related lipoatrophy. Fifteen patients in each of two arms are being given injections, one group at 0, 2 and 4 weeks; the other at 12, 14 and 16 weeks to evaluate the better time-lapse between injections. The results will be measured using facial ultrasound, photographs, visual assessments by patients and doctors, a health and depression questionnaire and blood counts. The results are due in March 2002.
New York plastic surgeon favours autologous fat transfer
New York plastic surgeon Jeff Brande, spoke to the meeting about autologous fat transfer, which is the transplantation of fat from elsewhere on the body. Dr Brande has 10 years of experience using this method as an anti-aging treatment and has been treating people with HIV-related lipoatrophy since 1996. A number of patients have been referred to him from the UK.
He said the method was to “gently tease” fat from the back or abdomen, ensuring that the fat cells remain intact, and then implant it into the face. He said the potential complications included bleeding and infections, as with any surgery, damage to veins, asymmetric irregularities and contour deformities, although he had not seen any of these. The surgery is usually performed under a general anaesthetic, although sometimes only a local anaesthetic is used. Some people suffer swelling for a week or 10 days. He said: “Patients usually want more fat.”
Dr Brande showed before and after pictures of the treatment and compared them to pictures of people who had had collagen treatment including a woman who had permanent red scars. He warned people: “I would stay away from collagen if I were you.” He also showed slides of people who had been treated with silicon – now illegal – that had fallen leading to sagging cheeks and buttocks, which now needed treatment. He said he now “distrusts” filler products.
Autologous fat transfer can only be performed on people with available fat elsewhere on their bodies. Dr Brande advised people: “If you have some body fat and your face is hollowing out, you should consider doing it earlier rather than later.”
So-called buffalo humps, which are large accumulations of fat between the shoulder blades and on the back of the neck, are widely reported in the US, although fewer cases have been reported in the UK. Dr Brande said he sees two or three people a week with this condition. Removing the fat from a buffalo hump can involve a two hour operation, he said.
Dr Youle said he did not know of anyone who is currently offering autologous fat transfer in the UK.
Personal accounts say the pain involved in PLA treatment is well worth it
Several people spoke about their experiences of treatment with PLA. John Stevens said: “It is painful. I chose to have an anaesthetic. It is like a load of little bee stings all over the face, but I didn’t care because I was so glad to have the treatment.” He compared it to other painful procedures and said having a tattoo or going to the dentist involved “far worse pain”. He said of the PLA injection: “It is just a tiny little prick.”
“After the treatment you massage the face for 24 hours,” he explained, “to make it smooth, or you can get lumps.” And he added: “It is not the perfect treatment, you are not going to look 21 again, and I do not look as I did four years ago. But I am so happy I had it.”
Another man told the meeting he paid £400 a session for three sessions of treatment with PLA in Harley Street. Elizabeth Laglenne commented: “That is too expensive.” The speaker added that the consultant at this clinic, Odile Brennan, then treated him twice more without further charge. He said he was delighted with the results of the treatment but thought it was wrong that he had had to pay. He said it was well worth the money but it was not right that it should only be available to those who could afford £1,200.
Amanda Cameron, who works for Medi-phill, the company that distributes New-Fill, said there were 30 to 40 professionals in the UK trained to provide the treatment.
The last person to speak at the meeting was Bernard Forbes of the UK Coalition of People Living with HIV and AIDS, who urged people to take part in the campaign to persuade the NHS to offer PLA treatment. He asked people to email Georgina Strutt at Camden and Islington Health Authority saying that she should include PLA in the Londonwide Treatment Strategy that she is currently preparing.
Information about New-Fill provided by Medi-phill Ltd
- It is biocompatible and biodegradable.
- It is immunologically inert.
- It has no animal origin.
- It has been used in medicine for 30 years for the encapsulation of vaccines and to carry slow-release medication for prostate cancer and infertility.
- It has been used in surgery for 30 years for resorbable (which means it can be broken down and assimilated into the body) orthopaedic implants, screws etc, and for resorbable sutures, as well as in skull and facial reconstructive surgery and tissue regeneration.
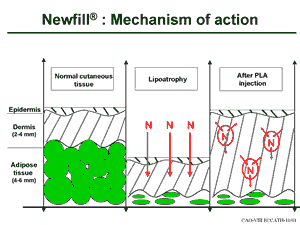
- It works in two ways: a) Immediate mechanical action related to volume, and b) Delayed reaction that results in the formation of new collagen, which persists despite resorption of PLA particles.
- It causes the proliferation of collagenous fibres that lead to natural dermal thickening.
- The fibres make up for the absence of fat layers and the skin ‘rises’ back to ‘normal’.
- The skin is soft and supple.
- It will be completely resorbed after three years.
- The result of treatment is that of neo-tissue which progressively diminishes.
- Repeat injections every three years are recommended by the manufacturers.
Comment
The clinician Odile Brennan and Medi-phill Ltd, distributors of New-Fill can be contacted on 020 7937 2377 or at their clinic at 40 Harley Street, W1G 9PP.
Copies of a full report of the i-Base meeting can be ordered by calling 020 7407 8488 or via our website,

